Translate this page into:
Transforming the emergency care scenario in India: A make in India approach
-
Received: ,
Accepted: ,
How to cite this article: Kandula VR, Taillac P, Nair R, Balasubramanya MA. Transforming the emergency care scenario in India: A make in India approach. Karnataka Med J 2023;46:24-7. doi: 10.25259/KMJ_5_2023
Situations like this are not uncommon in India and most other developing countries. Proper medical care in the ‘golden hour’ makes the difference between life and death, or between severe disability and complete recovery. Even though low- and middle-income countries (LMICs) pride themselves on some of the best hospitals and some like India attract medical tourists from around the world, access to reliable and quality emergency services has been grossly insufficient, especially at the grassroots.
Globally, traumatic injuries (22%), ischaemic heart disease which include neurological and cardiac emergencies (17%), lower respiratory infections (11%) and haemorrhagic strokes (7%) make up about 60% of emergency medical diseases. In addition, emergencies also occur during labour (postpartum haemorrhage, eclampsia and complications in newborn babies), among children and due to poisoning and envenomation.
Worldwide emergency medical diseases account for more than 50% of the disease burden and deaths. This proportion is higher in developing countries and there has been a 6% increase in overall mortality due to emergency medical disease from 1990 to 2015.[1]
Until recently, medical education has focused on making the right diagnosis with less emphasis on the principles of triage and emergency management. Although the medical curriculum includes a mandatory 2-week casualty rotation, there is no transfer of emergency care skills. Emergency care is offered in areas designated as ‘casualties’ that are often managed by junior specialty residents with little overview or by casualty medical officers who do not have special emergency skills training. Often, the casualty centres act as mere ‘referral points’ for specialized care. Hence, training in this setup does not equip young doctors with adequate skills to manage emergencies.
Many deaths due to critical illness are potentially preventable.[2,3] Several studies have documented that the basic life-saving clinical processes – Airway, Breathing and Circulation and focus on early recognition and prompt resuscitation may be overlooked even in specialised care centres and in both high[4-6] and low resources.[7,8]
A 2017 study of five urban university hospitals in India concluded that three out of five all trauma deaths were classified as preventable. The important areas of improvement identified were low-cost interventions such as airway management, fluid resuscitation, haemorrhage control and surgical decision-making protocols. The establishment of clinical protocols and timely processes of trauma care delivery is the next step towards improving care. The situation can be expected to be no better, if not worse at lower levels of health care.[9]
The inability to efficiently manage emergency patients has been leading to community rage, compromising the security of healthcare staff in the emergency department and the health infrastructure.[10] Poor staffing which includes inadequate training has been reported as a risk factor for violence against health-care team members in the emergency setting.[11] The lack of training among health-care personnel was further highlighted after the introduction of ambulance services (e.g., ‘108 ambulance’ systems in India). The ambulance services transport patients to the nearest healthcare facility in a timely manner. However, there has not been a commensurate improvement in the emergency management skills of health services personnel in most LMIC. A study in 2006 found that in LMIC even among doctors providing trauma care only a minority had taken Advanced Trauma Life Support or such other courses.[12]
An essential emergency and critical care (EECC) concept was devised through a Delphi process, involving a diverse panel of global clinical experts based on previous guidelines and the World Health Organization/International Committee for the Red Cross Basic Emergency Care. The group concluded that all levels of hospitals around the world have clinical processes and equipment to ensure early recognition and resuscitation of critically ill patients. Such readiness will ensure facing new challenges such as COVID-19 which may arise unexpectedly.[13]
In LMICs, it is unrealistic to expect patients in an emergency situation to be cared for by a health professional specially trained (e.g., postgraduate training) in emergency care. Most emergencies occur far from the tertiary hospitals in the community.
Hence, it is imperative that all doctors irrespective of whether they are generalists or specialists have a comprehensive set of skills to be able to provide quality emergency care during the ‘Golden Hour’. Thus, there is a need for comprehensive Emergency Care and Life Support training to equip all providers, irrespective of specialty, to Recognise, Resuscitate and when needed promptly Refer to a higher level of care. JeevaRaksha comprehensive emergency care and life support course (C-ECLS) empowers doctors to be proficient to deliver the EECC package of services which contains 40 clinical processes and 67 requirements, plus additions specific to COVID-19. This was evidenced by the confidence expressed by doctors who had undergone the ECLS course when they were caring for COVID-19 patients. For example, familiarity and confidence in handling different oxygen delivery methods and securing an airway.
The Medical Council of India has been suggesting that all medical colleges should train medical graduates on emergency care. Rajiv Gandhi University of Health Sciences (RGUHS) has initiated India’s unique 4-day ECLS course for doctors and a 3-day Emergency Nursing Life Support Course for nurses is being implemented for nurses as well. RGUHS has partnered with Swami Vivekananda Youth Movement, a nationally acclaimed Non-Governmental Organization working primarily at the grassroots. University of Utah, USA is the collaborating technical partner in this initiative [Figures 1 and 2].

- Scenario training.
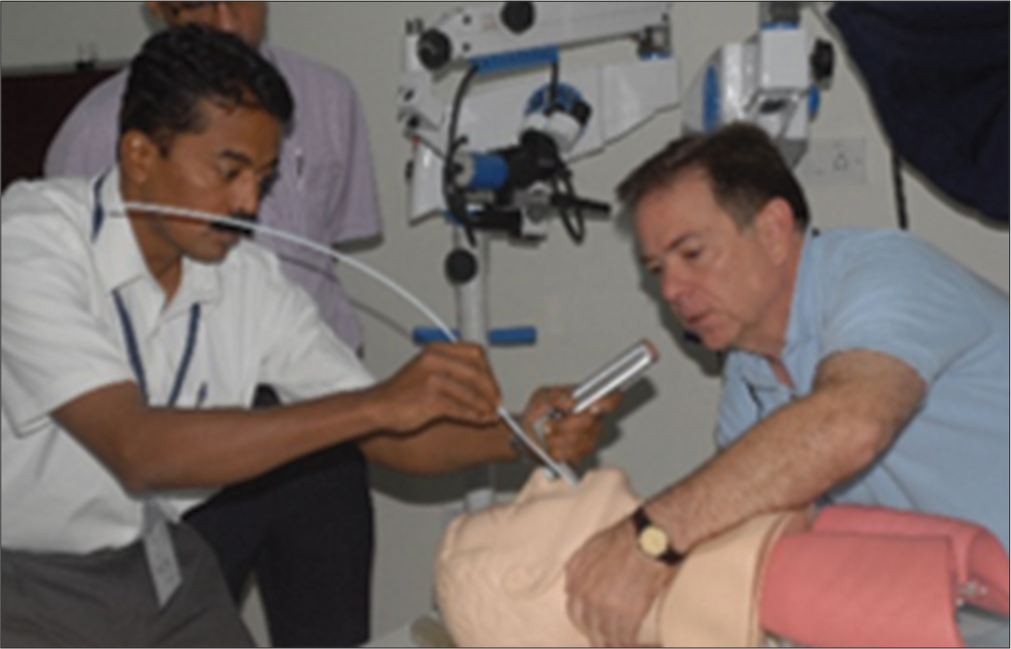
- Learning by doing: Securing airway.
The content from this course has been piloted across India through the National Health Systems Resource Centre, Ministry of Health and Family Welfare, Government of India which has recognised the efforts of RGUHS-JeevaRaksha TRUST [Figures 3 and 4]. The senior instructors from JeevaRaksha team have been invited and empanelled as Master Trainers and National trainers to roll out the emergency care and life support skills across the country.

- Scenario-based learning.

- Cardiopulmonary resuscitation (CPR) technique.
The Course was piloted in Morocco and Uzbekistan and implemented in Bhutan (2022). This confirmed our assessment that JeevaRaksha courses are equally relevant to the context of other LMICs. RGUHS-JeevaRaksha course has the potential to be exported to other states in India as a Karnataka model and to other developing countries as an Indian model [Figure 5].

- Learning skills in cadaver lab.
Ethical approval
The Institutional Review Board approval is not required.
Declaration of patient consent
Patient’s consent is not required as there are no patients in this study.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Global, regional and national burden of emergency medical diseases using specific emergency disease indicators: Analysis of the 2015 Global Burden of Disease Study. BMJ Glob Health. 2019;4:e000733.
- [CrossRef] [PubMed] [Google Scholar]
- The impact of early monitored management on survival in hospitalized adult Ugandan patients with severe sepsis: A prospective intervention study. Crit Care Med. 2012;40:2050-8.
- [CrossRef] [PubMed] [Google Scholar]
- Improved triage and emergency care for children reduces inpatient mortality in a resource-constrained setting. Bull World Health Organ. 2006;84:314-9.
- [CrossRef] [PubMed] [Google Scholar]
- Preventable deaths due to problems in care in English acute hospitals: A retrospective case record review study. BMJ Qual Saf. 2012;21:737-45.
- [CrossRef] [PubMed] [Google Scholar]
- Confidential inquiry into quality of care before admission to intensive care. BMJ. 1998;316:1853-8.
- [CrossRef] [PubMed] [Google Scholar]
- Unexpected death within 72 hours of emergency department visit: Were those deaths preventable? Crit Care. 2015;19:154.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluating the impact of pulse oximetry on childhood pneumonia mortality in resource-poor settings. Nature. 2015;528:S53-9.
- [CrossRef] [PubMed] [Google Scholar]
- Unmet need of essential treatments for critical illness in Malawi. PLoS One. 2021;16:e0256361.
- [CrossRef] [PubMed] [Google Scholar]
- Learning from 2523 Trauma deaths in India-opportunities to prevent in-hospital deaths. BMC Health Serv Res. 2017;17:142.
- [CrossRef] [PubMed] [Google Scholar]
- Violence against physicians and nurses: A systematic literature review. J Public Health (Berl) Z Gesundh Wiss. 2022;30:1837-55.
- [CrossRef] [PubMed] [Google Scholar]
- Violence in the emergency department. Psychiatr Clin North Am. 2016;39:557-66.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluation of trauma care capabilities in four countries using the WHO-IATSIC guidelines for essential trauma care. World J Surg. 2006;30:946-56.
- [CrossRef] [PubMed] [Google Scholar]
- Essential emergency and critical care: A consensus among global clinical experts. BMJ Glob Health. 2021;6:e006585.
- [CrossRef] [PubMed] [Google Scholar]





